Payment rules
A rundown of 2022 Medicare Physician Fee Schedule
Isabelle Bibet-Kalinyak //January 24, 2022//
Payment rules
A rundown of 2022 Medicare Physician Fee Schedule
Isabelle Bibet-Kalinyak //January 24, 2022//

The Centers for Medicare & Medicaid Services recently released its 2022 Medicare Physician Fee Schedule. The MPFS Final Rule, which took effect on Jan. 1, aims to advance CMS’ strategic commitment to drive innovation to support health equity and high-quality patient-centered care.
The MPFS Final Rule appears broad and ambitious on the surface, but many of the progressive changes publicized by CMS remain limited to very narrow circumstances as highlighted below.
Evaluation/Management Visits
In consideration of the evolving role of non-physician practitioners, Medicare is defining “split or shared” E/M visits as E/M visits provided in the facility setting by a physician and an NPP in the same group. The visit is billed by the physician or the NPP who provides the substantive portion of the visit. For 2022, the “substantive portion of the visit” can be history, physical exam, medical decision-making, or more than half of the total time (except for critical care, which can only be more than half of the total time). By 2023, the “substantive portion of the visit” will exclusively mean more than half of the total time spent. The individual who performs the substantive portion must sign and date the medical records. The MPFS Final Rule also defines when critical care services can be billed concurrently with E/M visits and surgical procedures and how services furnished by teaching physicians involving residents can be billed.
Telehealth
The MPFS Final Rule expands the use of telehealth by adding to the definition of “interactive telecommunications system for telehealth services” audio-only communications technology for the diagnosis, evaluation, or treatment of mental health disorders under certain circumstances. The rule applies broadly to mental and behavioral health services such as psychiatric services, counseling, therapy services, treatment of substance use disorders, and services provided through Opioid Treatment Programs. Medicare permits and pays for remote access to mental and behavioral health services via audio-only telephone calls from the patient’s home when the beneficiary is not capable of, or does not consent to, the use of two-way audio/video technology, and provided some in-person non-telehealth visits take place within set frequency. Medicare will also pay for mental health visits furnished by Rural Health Clinics and Federally Qualified Health Centers via telecommunications technology.
Diabetes Prevention
MDPP suppliers provide structured, coach-led sessions in community and health care settings using a Centers for Disease Control and Prevention-approved curriculum to provide training in dietary change, increased physical activity and weight loss strategies. To boost access to MDPP suppliers for Medicare beneficiaries living in rural areas and decrease the number of individuals with type 2 diabetes in both urban and rural communities, CMS is taking steps to improve its MDPP expanded model, which was developed to prevent Medicare beneficiaries with prediabetes from developing type 2 diabetes. CMS is waiving the Medicare enrollment fee for all organizations that apply to enroll as an MDPP supplier, shortening the MDPP services period from two years to one, and restructuring payments so MDPP suppliers receive larger payments for participants who reach milestones for attendance.
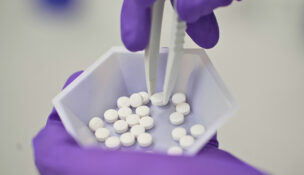
Vaccine Administration
To promote access to safe and effective vaccines, the MPFS Final Rule nearly doubles the payment rates for influenza, pneumococcal, and hepatitis B vaccine administration from approximately $17 to $30, while maintaining the current payment rate of $40 per dose for the administration of the COVID-19 vaccines.
Payment System
The MPFS Final Rule implements multiple key changes to the Medicare Quality Payment Program, the value-based payment regime that promotes the delivery of high-value care by clinicians through a combination of financial incentives and disincentives. It raises the MIPS performance thresholds that clinicians must exceed to be eligible for positive payment incentives in 2022. It also introduces the first seven MIPS Value Pathways, subsets of connected and complementary measures and activities that providers can report on to meet MIPS requirements: rheumatology, stroke care and prevention, heart disease, chronic disease management, lower extremity joint repair such as knee replacement, emergency medicine and anesthesia. MVPs are designed to improve patient outcomes by more effectively measuring and comparing performance within different specialties and providing clinicians more meaningful feedback. In addition, the MPFS Final Rule revises the current definition of “eligible clinician” to include clinical social workers and certified nurse-midwives among those participating in MIPS to incentivize high-quality care for professionals that are often a key point of contact for underserved communities with acute health care needs.
Physician Assistant Services
PAs can bill Medicare directly for their personally performed professional services, reassign payment for their professional services, and incorporate with other PAs (subject to applicable state laws). This important change grants PAs the same rights as nurse practitioners who have long been able to bill Medicare directly for their services.
As always with the Medicare rules, providers need to analyze the new changes in context and in great detail to ensure that they satisfy all the requirements, and, most important, understand how to document said requirements in the medical records to prevent claim denials and costly repayments to CMS.
Isabelle Bibet-Kalinyak is a member at Brach Eichler LLC.